Where Breastfeeding Advocates Get it Wrong
Have you ever wanted to give your child the best and couldn’t? What if the best was something that 99% percent of mothers could give but you couldn’t? For me, this happened very early on in motherhood: I couldn’t produce enough milk to feed my first child, my son Rocco. Only 16 months after my son Rocco was born, the breastfeeding anxiety has returned with the birth of my daughter Giada last month.
Breastfeeding advocates fail to acknowledge that not all women are physically able to breastfeed. They push “breast is best” so hard, that not being able to produce enough milk made me feel horrible about myself and figure I must be doing something wrong. If I don’t breastfeed — because of course all mothers can — then I must be lazy, selfish, ignorant, a quitter or don’t really care about my child’s health, right?
Having an issue with milk production right in the middle of a major resurgence in breastfeeding advocacy is a cruel irony. The American Academy of Pediatrics strongly encourages mothers to breastfeed exclusively for the first year of life. Waiting rooms and doctors’ offices brim with educational materials that promote breastfeeding. My own prenatal care included breastfeeding preparation classes and offered discounts on breast pumps and other breastfeeding paraphernalia.
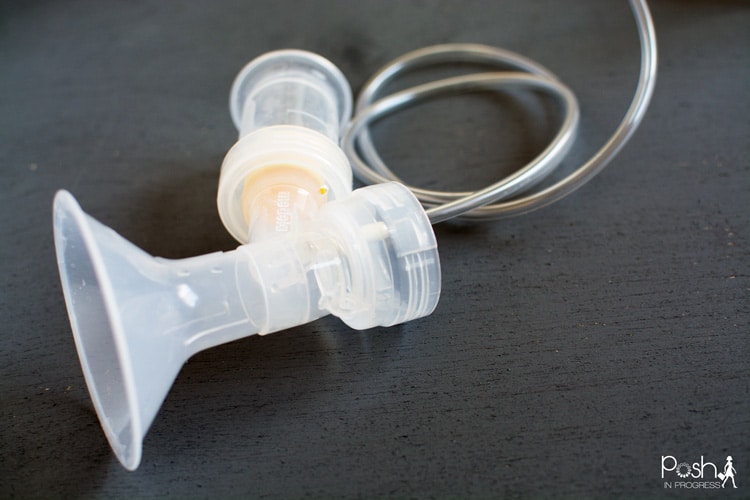
I tried my nipples off, almost literally. I pursued every course of action to sustain breastfeeding exclusively. I had undersupply issues with my son, so I had to use an industrial strength, hospital grade breast pump that mechanically tugged and pulled at tender parts of my body for 20 minutes, every two hours (including the middle of the night) for six weeks.

Beyond spending the first six weeks of motherhood sleep deprived, practically topless and strapped to a breast pump, the machine removed layers of sensitive skin, which caused my nipples to bleed and develop sores. All that pain and effort only produced single-digit milliliters of breast milk each session, which was a literal drop in the bottle, compared to how much he actually needed to survive.
Despite my resolve, my body let me down and no one knew exactly why. I, most likely, have insufficient glandular tissue to produce an adequate supply, or it was because of my thyroid issues. But the fact remained that no amount of intervention would make nursing sustainable for me.
I was devastated. I cried countless times; I was a failure. I had let my son down (even as I type this, I have tears in my eyes remembering the painful feelings of inadequacy and not being able to provide the best nutrition for my son). It took me a very long time to come to terms with my inability to nurse my son. I still feel badly about it. My feelings of disappointment only stronger because of the media and medical community’s stance that breastfeeding is the only viable option.
If it’s not evident by my pumping experience, I am completely pro-breastfeeding. I absolutely buy into the fact that women’s bodies are designed to nurse and provide food for their children. I also agree that many women give up too quickly and don’t put in the hard work required to nurse exclusively, so I can understand why lactation consultants and doctors work so hard to promote breastfeeding. It is their job, and they only want the best possible health for our children.
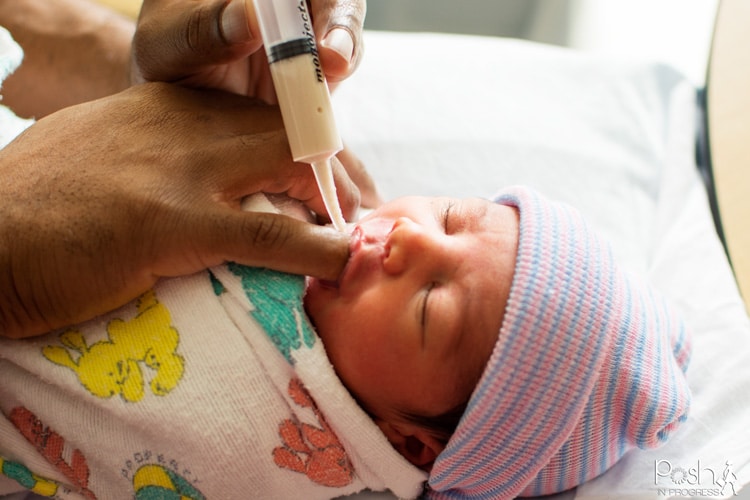
But what about those of us who try our darnedest, who have sore and bleeding nipples due to latching issues, who pump every two hours for weeks on end, who visit their doctors to ask for medical interventions and medications to help, who feed their babies through syringes to avoid nipple confusion, who visit the lactation consultants weekly, but just can’t increase our supply?
It has been my experience that women like me, who truly can’t produce an adequate supply, are met with accusatory questions and misunderstanding. There is an overarching belief that all women should be able to breastfeed, when in fact, there are indeed, women who simply can’t. Yes, it is rare that women who put in the hard work are not able to increase their supply, but it does happen.
The problem is, we are the exception, not the rule. The other issue is there is very little research and support for the small percentage of women who cannot breastfeed (statistically only 1 in 1000 women will have insufficient glandular tissue, but 15% fall into the category of lactation failure).
When I found out I was pregnant with my second child, I steeled myself knowing I probably would not be able to breastfeed her. My doctor and lactation consultant encouraged me to try again. They told me every pregnancy is different because your hormones change with each pregnancy. Although, they reluctantly agreed I most likely would have difficulty again.
I decided to try to breastfeed my daughter, but I would not put myself through the same level of personal torture that I had the first time around. My failed attempts with Rocco took an emotional and mental toll on me that was unhealthy. Ironically, my frenetic breast pumping efforts, working to be a good mother, cost me precious bonding time with my baby boy and scarred my first weeks of motherhood.
A month ago, we welcomed my daughter and it was déjà vu all over again. My motherly instincts shouted down all of my tormenting breastfeeding memories. As if on cue, within a couple hours of her birth, the breastfeeding propaganda kicked into high gear.
My concerns about my ability to breast feed again seemed to fall on deaf ears. I imagine this is because doctors and lactation consultants see hundreds of women a year and much of what they advise is rote regurgitation. It felt as though they were waiting for me to finish expressing my fears so they could go through their checklist. The doctor’s and lactation consultant’s exhibited an all-knowing attitude and their dismissive responses to my comments brimmed with judgment, questioning the vigor of my past efforts.
Granted, every pregnancy is different and I didn’t know for a fact that I wouldn’t be able to feed my daughter, but wouldn’t a more compassionate approach that recognized my struggles better muster enthusiasm for a second try than a sugar-coated brow beating?
Regardless, I decided to pump again while in the hospital because it wasn’t about me, it was about my daughter and what was best for her. Instead of bonding with my new daughter and resting, her first day of life I spent pumping. My anxiety grew with each sad little trickle of milk, trying to fill those bottles by force of will.

By the second week, my anxiety and feelings of insecurity reached a breaking point and I decided all of this concentration on pumping had to stop. I had seen an increase in production from my experience with Rocco, but the totals were still far less than the equivalent of a quarter of a meal for my daughter.
Doctors and lactation consultants met my decision with silence and disappointed looks. Despite their reactions, I finally stopped caring about their approval and enjoyed the precious first moments with my daughter.
Another irony, when I let go of other people’s expectations and did what was right for me, what allowed me to be the most emotionally and mentally stable, my supply increased. Although I still can only produce about 10% of her dietary needs, I am producing about five times as much milk as I did with my son.
At times (especially as I write this story) I am flooded with feelings of inadequacy and disappointment for my inability to breastfeed my children exclusively, as I envisioned. As I watch both of them grow healthfully, I am reassured that my inability to breastfeed is not the measure of my worth as a mother.
I am fortunate I was able to experience nursing my son and daughter. Even if I was never able to fully sustain the practice, I was able to give them some colostrum and breast milk, and feel what it is like to bond with my children through nursing.
By sharing my difficulties, I hope this story brings awareness to those of us who are physically unable to breastfeed exclusively. I want the medical community not to dismiss us, not to contribute to making us feel guilty, but rather to help us find solutions and interventions. Although I suspect my issue is at least partially genetic, I hope the medical community will take a closer look at women with underproduction issues to find a solution so that my own daughter doesn’t have to deal with this some day.
For those of you who have experienced difficulty with breastfeeding: undersupply, oversupply, latching issues, mastitis, you are not alone. Breastfeeding advocates, take note. We appreciate your enthusiastic belief and support of breastfeeding, but don’t forget about us. There are those of us who simply cannot sustain breastfeeding, and rather than your accusatory stares or comments, we need your support and comfort.






